AUSTIN, Texas—Involving geriatricians in the pre- and postoperative care of older patients undergoing abdominal wall reconstruction can lead to a meaningful improvement in many outcomes, according to new research.
A few years ago, researchers at Atrium Health Carolinas Medical Center, in Charlotte, N.C., identified predictors of increased length of stay (LOS) in patients undergoing AWR. “Unfortunately, we found that most of these factors, including age, were not modifiable in our patients. But then we thought, maybe we could modify age by involving our geriatricians in a preoperative clinic,” said Hadley Wilson, MD, a surgical resident at the Carolinas Medical Center.
To assess whether including geriatricians in the care of their older patients had any benefits, Dr. Wilson and his colleagues conducted a prospective observational cohort study comparing outcomes before and after the inclusion of geriatrician evaluation in older patients undergoing AWR at their tertiary hernia care center.
“What geriatricians do in the clinic is a comprehensive geriatric assessment; the emphasis is on function and optimizing the patient’s functional status before surgery,” Dr. Wilson said. In addition to evaluating geriatric syndromes like memory loss, falls, hearing impairment, vision loss, anxiety and depression, geriatricians also help with medication management and the avoidance of polypharmacy.
Further, geriatricians evaluate these patients after surgery, monitoring for the onset of delirium and helping in the postoperative plan for support, ensuring patients and their families are prepared for discharge to home, he said. “Perhaps most importantly, they help manage expectations preoperatively as far as what patients can expect in their recovery and how they can expect to improve,” Dr. Wilson said. “And they are very useful in our patient selection, perhaps steering some patients who didn’t understand how the surgery might affect them physiologically and mentally and their independence.”
Dr. Wilson and his colleagues retrospectively propensity-matched patients who had undergone geriatrician evaluation with those who had surgery before that intervention, matching on age, hernia type, and comorbidities such as diabetes, body mass index and chronic obstructive pulmonary disease. Their outcomes included surgical complications, composite medical complications (e.g., cardiac complications, respiratory failure, deep vein thrombosis, sepsis and pneumonia), ICU admissions and LOS.
Since the implementation of geriatrician evaluation, 160 patients have seen these specialists and undergone surgery at the medical center. The patients average 74 years of age, a slight majority (55%) are female and they average nearly five comorbidities per patient.
“After propensity matching, we had 124 patients in each group. Outcomes showed a three times’ reduction in complications overall in patients who saw geriatricians and a seven times’ reduction in ICU admissions,” Dr. Wilson said. In addition, patients who saw a geriatrician had a shorter hospital LOS, by two days on average.
Seeing that the largest proportion of patients were undergoing surgery for ventral hernia repair, they did a subgroup analysis comparing only those patients. They saw a reduction in medical complications, of 2.4 times, and again a sevenfold reduction in ICU admissions.
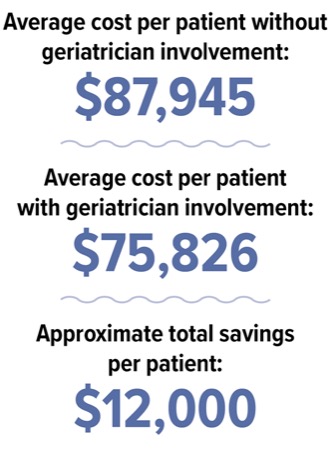
Despite the additional consultation and possible charge for geriatrician care in the hospital, the reductions in complications, LOS and ICU admissions added up to a substantial cost savings. Before geriatrician involvement, the average charge for each patient was $87,945, compared with $75,826 for patients who saw a geriatrician, an average total charge savings of more than $12,000.
The researchers did not see recurrences in either set of patients, but acknowledge they had a fairly short follow-up period: 22 months for the non–geriatrician-evaluated group and 6.8 months in those evaluated by a geriatrician.
Dr. Wilson said that by lowering complications and reducing LOS, geriatrician evaluation can help improve resource utilization at their institution and others like it. “Tertiary hernia centers and other surgeons who perform complex operations should consider geriatric prehabilitation with geriatric specialists,” he said.
Dr. Wilson presented his research at the 2023 meeting of the American Hernia Society and was awarded the Bassini Award for the best overall research presentation at the conference.
Courtney Collins, MD, a clinical associate professor of surgery at The Ohio State University, in Columbus, said that since surgical patients in general are getting older, with hernia repair being the most common elective operation in the United States, it is crucial that surgeons optimize their practice around this high-volume and vulnerable patient group.
“Surgeons are often ill-equipped to deal with the physiologic and psychosocial complexities their older patients present with. As this work shows, these older adults can greatly benefit from the input of specialists. Geriatricians can, in some instances, help optimize patients before surgery, but crucially then can also help ensure older patients get the appropriate post-discharge care and education,” she said.
Dr. Collins also observed that while a geriatric consult can seem like “just one more thing” standing between the surgeon and an operation, it can help prevent expensive and potentially devastating complications.
This article is from the May 2024 print issue.


Please log in to post a comment