‘That which we call a rose
By any other name would
Smell just as sweet.’—William Shakespeare, “Romeo and Juliet”

Remarkably, 8,000 or so medical eponyms—diseases, syndromes, procedures, rules—are named after a person or a place. Using these names to describe them has become a lingua franca of medicine and science. Identification by a person’s name is generally considered as honoring that individual.
The eponym tradition has been the subject of over 25 books, as well as several dictionaries of eponyms. However, the use of eponyms has been condemned by prestigious medical groups who have advised eliminating them from the medical lexicon. In 1974, the National Institutes of Health recommended refraining from the use of possessive eponyms. In 1975, in the Lancet, the Canadian National Institute of Health stated, “The possessive use of an eponym should be discontinued, since the author neither had nor owned the disorder.” In 2004, the World Health Organization advocated for the elimination of medical eponyms; in 2007, the American Medical Association followed suit.
Yet, we continue to use eponyms, create new ones and will probably do so in the future. They have a certain attraction as a shorthand for communication; they are a private language for the initiated. At the same time, eponyms can be misleading, erroneous, incorrectly attributed and, possibly, pose obstacles to progress by implying knowledge when there actually is ignorance.
Some Well-Known Eponyms
Crohn’s Disease
This “disease” was described in JAMA in 1932 by Crohn, Ginzburg and Oppenheimer (1932;99:1323-1329). Crohn was a gastroenterologist, Ginzburg a surgeon and Oppenheimer a urologist. Although Crohn was the senior of the three, all of them should have received eponym credit, especially Ginzburg, the surgeon, who first visualized the characteristic pathology in the OR. Such an eponym, however, would have been a mouthful. Crohn’s disease is actually a conglomerate of clinical and pathologic descriptions. Can Crohn’s, therefore, realistically be termed a disease? Nearly 100 years after its emergence as an entity, no specific etiology has been ascertained. At one time, it was believed and actually taught in medical schools that Crohn’s, first described at the Mount Sinai Hospital of New York, was a disease found in young Jewish girls who were morbidly dependent on their mothers. When I first came to Minnesota and examined a laconic Swedish farmer with classic Crohn’s, I was tempted to tell him that he must actually be a young Jewish girl overly attached to his mother.
Alzheimer’s Disease
The condition was first described by Dr. Alois Alzheimer, a clinical psychiatrist and neuroanatomist, in 1906, in a report of a single patient, a woman with memory loss, language problems and unpredictable behavior. In his description of this syndrome, he emphasized that it was a specific type of dementia in individuals under the age of 65 years. Today, however, the diagnosis of Alzheimer’s is also commonly made for dementias starting after age 65. Characteristic brain changes of Alzheimer’s of cell death, amyloid deposits, neurofibrillary tangles, chronic inflammation and glial cell dysfunction are found in many of the at least 30, possibly over 100, dementias described in the literature (in essence, comparable to naming warts by their location, color, size, etc.). And, the etiology, the true genesis of Alzheimer’s, remains unknown. Is Alzheimer’s, therefore, even a unique disease? Finally, to be accurate, Alzheimer himself defined his case study as “pre-senile dementia”; it was Emil Kraepelin, who, in 1910, gave the syndrome its name to honor Alzheimer, who was his pupil. Incidentally, a similar clinical dementia symptomatology, Lewy body dementia, diagnosed in the late actor Robin Williams, wherein the brain shows certain structural changes, was first described by Dr. Fritz J.H. Lewy, who worked in the laboratory of Dr. Alzheimer as his student.
Down Syndrome
First described by John L. Down, in 1866, Down syndrome is one of the few medical eponyms with a known etiology, elucidated by Jerome L.M. Lejeune in 1959, as an extra chromosome 21, also referred to as trisomy 21. This knowledge should warrant changing the name to Down-Lejeune disease, because it is an actual disease entity—a rarity in the language of eponyms.
Peyronie’s Disease
First observed in 1561 by Gabriele Fallopius and Andreas Vesalius, it was fully described, in 1743, by Francois Gigot de la Peyronie. It is stated that Peyronie had a lifelong obsession with the male phallus; today, he might take pride in having his name attached to it. The etiology of this not-uncommon (4% or greater occurrence in U.S. males and likely underreported) fibrosis of the penis is unknown, and, again, may properly be described as a syndrome but not as a disease.
Nazi Eponyms
There are powerful advocates for renaming and thereby dishonoring the named contributions of confirmed Nazis. Among these 30 or so eponyms are Asperger’s syndrome (an autism disorder), Reiter’s syndrome (reactive arthritis) and Wegener’s granulomatosis (granulomatosis with polyangiitis). Particular attention has been paid to the Clara cells, a population of nonciliated bronchial epithelial cells that protect the airway from environmental toxins. Max Clara was an outspoken member of the Nazi party who conducted his research on the lungs of prisoners he selected prior to their execution. He expressed his affection for Nazism in an introduction to an academic directory by stating, “this science has contributed to the great plans of the FÜhrer.”
Honorific Eponyms That Should Be Given For Contributions to Medicine
Hippocrates’ Syndrome: Obesity and Sequelae
Hippocrates (460-370 b.c.) said, “Corpulence is not only a disease itself, but the harbinger of others,” a truth not as well articulated for the next 2,500 years. Hippocrates described many of today’s common diseases but is best remembered for the Latin translation from the Greek of “primum non nocere” (“first, do no harm”), falsely attributed to the Hippocratic Oath, but actually part of his “Of the Epidemics.”
Aretaeus of Cappadocia Syndrome: Diabetes
In a.d. 150, possibly based on the 1552 b.c. writings of Hesy-Ra, an Egyptian physician, Aretaeus coined the term diabetes to describe “the melting down of flesh and limb into urine.”
Leonardo da Vinci Syndrome: Coronary Arterial Atherosclerosis
On dissecting the “centurion,” a 100-year-old man in 1508, da Vinci diagnosed the cause of death to be “clinkers in the veins of the heart that choked the life-force out of it.” This was at a time before arteries and veins were clearly distinguished and before Harvey’s description of the circulation of blood in 1618.
Marshall–Warren Disease: Peptic Ulcers
Peptic ulcers, gastric and duodenal, have been described since antiquity. Linked to hyperacidity, 20th-century therapy consisted of a diet high in cream, milk and eggs (the “Sippy Diet,” named after Bertram W. Sippy, 1866-1924), which is possibly one of the causes for the 20th-century increase in atherosclerosis. Twentieth-century medical teaching erroneously theorized that ulcers occurred in mid-level executives frustrated in their efforts to ascend in their companies. When I came to the Midwest, I could have written a paper stating that peptic ulcers can also be found in autonomous farmers worried about their crops. In 2015, Drs. Barry Marshall and Robin Warren were awarded the Nobel Prize in Physiology for demonstrating that peptic ulcers were caused by the bacterium Helicobacter pylori. These Australian physicians observed H. pylori in ulcer patients and cultured the organism, followed by its self-administration by Dr. Warren, who developed classic peptic ulcer symptomatology, from which he was cured by antibiotic therapy, thereby fulfilling Koch’s postulates (1890) for the definition of a disease. I doubt that peptic ulcer disease will ever receive the deserved Marshall-Warren eponym.
Semmelweis Procedure: Handwashing
For whimsy, let us consider one more unawarded eponym: handwashing before tending to a patient, the concept for which in 1846 Ignaz B. Semmelweis was ostracized, dismissed from his institution, declared insane and died after being whipped in an “insane asylum.” When you next go to the OR, honor him by saying, “I am going to do a Semmelweis.”
Should We Continue to Use Eponyms?
Using an eponym to describe a disease implies that we know its cause and understand its processes. If we don’t, using the eponym is like using the adjectives, idiopathic, primary or essential, instead of “I don’t know.” Using an eponym as the correct name for a disease is justifiable for Marshall-Warren disease but not justified for Crohn’s, Alzheimer’s, Lewy body dementia, and many other symptom complexes or related pathologic findings for which currently there is no known etiology or metabolic mechanism justifying designation as a disease.
Future investigators have a great opportunity: They can research diseases named by eponyms, elucidate their origins and discover therapy for their mitigation. Such science could eliminate old eponyms, substitute new ones or discard eponymization altogether.
Buchwald’s Rule
Before eponyms are eliminated, let me add “Buchwald’s Rule”: Don’t trust eponyms.
Dr. Buchwald is professor emeritus of surgery and biomedical engineering, and the Owen H. and Sarah Davidson Wangensteen Chair in Experimental Surgery, at the University of Minnesota, in Minneapolis. His articles appear every other month.
This article is from the April 2023 print issue.


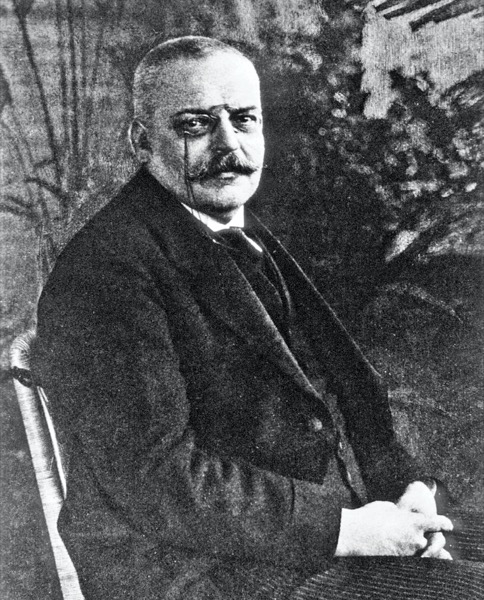
Please log in to post a comment