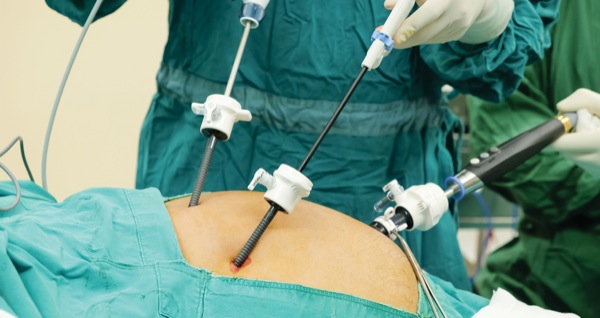
Boston—When laparoscopic cholecystectomy was introduced a generation ago, the procedure revolutionized the task of surgically removing a troublesome gallbladder. For most patients, the “lap chole” eased discomfort after surgery, leading to a short hospital stay or, more commonly, an outpatient procedure.
But lap choles also created a significant problem from the outset: a higher number of bile duct injuries (BDIs) than open cholecystectomies. The problem persists, as the rate of BDIs has remained constant despite years of surgical experience with lap choles. BDIs are costly to both the affected patients—some of whom die or see their quality of life diminish when they had been otherwise healthy—and the surgeons and their institutions, who have to pay for medicolegal bills.
The issue has been a simmering one for surgeons who specialize in the procedure. To address this problem, nearly 200 surgeons, physicians and others from across the United States gathered last October for a summit on developing ways to reduce BDIs.
The Multi-Society Prevent BDI Consensus Conference brought together five top surgical societies and gastrointestinal surgeons from around the world to review challenges and develop strategies to cut the number of BDIs or manage them when they happen. They discussed matters such as whether to perform a cholecystectomy within 72 hours of inflammation in acute cholecystitis, how best to use imaging, and when to refer to an expert in the event something goes wrong.
The five surgical societies were the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES), the Americas Hepato-Pancreato-Biliary Association (AHPBA), the International Hepato-Pancreato-Biliary Association, the Society for Surgery of the Alimentary Tract, and the European Association of Endoscopic Surgery.
“We really think that this is going to carry a lot of weight in the surgical world, and will help set guidelines that are useful for surgeons in practice,” said L. Michael Brunt, MD, the chief of minimally invasive surgery at Washington University School of Medicine in St. Louis. “The problem has not gone away. We as a surgical community can do better in terms of our education and our outcomes.” Dr. Brunt, the conference’s lead organizer, said he was especially impressed by the amount of concordance at the meeting about how best to attack the problem.
A Surprisingly Common Complication
Dana Telem, MD, an associate professor of surgery at the University of Michigan, in Ann Arbor, outlined the seriousness of BDIs. Lap choles are among the most common operations in the United States, she said, with between 750,000 and 1 million performed each year. Complications arise in about 7% of patients, including bleeding, abscess and leaks. Although only 0.4% results in BDIs—the most dreaded complication—that translates to about 3,000 injuries per year.
“This has a major effect on health resource utilization,” said Dr. Telem, who was also a conference planner. Up to 10% of patients require treatment in the emergency department, and up to 7% require hospital readmission, “which is a little bit high considering that this is an outpatient procedure,” she said. In addition, “we’re not seeing improvement over time. It’s not an issue of ‘well, once we get our skill set up things are going to get better; they’re going to improve.’ They haven’t.”
Dr. Telem cited a comprehensive Swedish national registry of 51,041 patients—a fount of data for research into BDIs—that found 1.5% of people having a lap chole ended up with an injury and 0.34% had a major BDI that required reconstructive surgery.
She discussed the societal impact of these BDIs. They result in $1 billion a year in associated costs, she said, half of which were legal expenditures. “It’s actually the number one litigated case against surgeons. If you think about all the operations that all of us do, 20% of the malpractice claims are just around this common procedure.”
Mortality rates within 10 years of patients having suffered a major BDI are also 20.8% higher, Dr. Telem said. “These patients oftentimes don’t do well. They need numerous reinterventions, hospitalizations. There’s early and late complications.” Even for patients who are physically all right in the long run, “there’s still an emotional toll,” she said. Scores on long-term quality of life are lower, in part because patients are readmitted and cannot work, while still having out-of-pocket expenses. “Can you imagine going in for a lap chole and coming home with $300,000 in medical bills after a procedure, and how that would impact or perhaps financially ruin people? So it’s not surprising that we’re seeing the anger.”
Steven Strasberg, MD, a professor of surgery also at Washington University School of Medicine in St. Louis, noted that the rate of BDIs was about one in 1,000 in the open era, about one-third of the rate in the laparoscopic era. He warned against “drawing conclusions” from studies on BDIs that have few patients because it “may give the illusion of safety.”
Steps Moving Forward
After addressing the urgency of the issue, the conference turned to a series of questions, divided into sections: prevention, disease, patient factors and actions to limit the risk and severity of BDIs. The objective of these questions was to develop optimal strategies for evidence-based guidelines, which were voted on by an expert panel of 25 surgeons. Recommendations were approved if 80% voted in favor. Other physicians in attendance also were allowed to cast votes.
One of the key recommendations concerned whether a lap chole should be done immediately—within 72 hours of symptom onset—or up to six weeks after a patient experiences acute gallbladder inflammation. Experts suggested that those with mild acute cholecystitis get the procedure within 72 hours of symptom onset, but there was insufficient evidence to make a recommendation for patients with moderate or severe inflammation. The experts also suggested that studies examining the link between BDI and acute inflammation should match patients at baseline on both inflammation severity and a history of previous bouts of cholecystitis. Previous attacks of inflammation “are associated with an increased risk of injury,” Dr. Strasberg said. “They’re usually [in] men.”
Several recommendations involved imaging during a cholecystectomy. One urged that in patients with uncertain biliary anatomy, or if there is a suspicion that a BDI occurred during a procedure, that surgeons use intraoperative techniques—notably cholangiography—to reduce the risk for a BDI. (A study based on the comprehensive Swedish Registry for Gallstone Surgery, known as GallRiks, found that intraoperative cholangiography decreased the risk for BDI in patients who had acute cholecystitis or a history of acute cholecystitis.)
Surgeons with lap chole experience may use ultrasound as an alternative to cholangiography. However, some surgeons, notably those from countries outside the United States and rural areas, said their institutions don’t have the proper imaging devices like ultrasound. Charles Vollmer Jr., MD, the president of the AHPBA and director of pancreatic surgery at Penn Medicine, in Philadelphia, cautioned that there’s “an art” to interpreting the images. Without the ability to interpret, he said, “what do you do when you get in trouble?”
With these recommendations, the panel also discussed whether surgeons should use video or photography in addition to written documentation in the operative note. Questions arose, however, as to how best to capture those images. One doctor questioned whether a smartphone would suffice; another spoke of outdated VHS tapes stored at his institution; and still another worried that images can be a double-edged sword in the event of legal action after a procedure goes badly.
“We have to get over the legal fear,” said Marian McDonald, MD, a general surgeon at St. Luke’s University Health Network in Allentown, Pa. Dr. Brunt asked about using photodocumentation during surgery: “Doesn’t it drive you to do a little bit better job?”
Better Surgical Techniques
Among aspects of surgery, the experts agreed that a multiple-port laparoscopic technique is better than a single-port, single-incision one to mitigate BDI risk.
They also agreed that currently there isn’t enough evidence to recommend whether to convert from a lap chole to an open one to limit or avoid a BDI. “We know there are bad outcomes and bad repairs,” Dr. Vollmer said. Experts noted that some young surgeons don’t have much experience with an open procedure. In the absence of current evidence, the experts called for prospective and retrospective comparisons of clinical outcomes for “bailout” options.
There was disagreement about whether surgeons should take a time-out to verify the critical view of safety to reduce the risk for BDI. Some even queried what even qualified as a time-out. A recommendation that surgeons take a time-out did not pass.
Demetrius Litwin, MD, a general surgeon at UMass Memorial Medical Center, in Worcester, said it was a good idea to “pause before you irreversibly cut or clamp.” However, some attendees asked who in the OR had the skill set or ability to contradict what the surgeon was doing. “No one has more skin in the game than the surgeon,” one attendee said.
“[Except perhaps] the patient,” replied Nathaniel Stoikes, MD, a general surgeon at the University of Tennessee, in Memphis.
When a BDI does occur during a lap chole, the experts recommended that surgeons refer the patient quickly to a surgeon experienced in handling such an injury, and preferably at an institution with a hepatobiliary specialty team. Referral “implies good judgment, not failure,” said Horacio Asbun, MD, the chair of general surgery at Mayo Clinic in Jacksonville, Fla., who urged a “fast-track” referral and to avoid doing anything that would worsen the situation. It is a good idea both medically and legally, he said, adding, “This is going to help the surgeon in the courtroom” in the case of a malpractice suit. Nathaniel Soper, MD, the chair of surgery at Northwestern Medicine, in Chicago, said surgeons could use video calling to consult an experienced one elsewhere. Without such guidance, he said, “I think you can have really bad judgment in that situation.”
Keith Lillemoe, MD, the chief of surgery at Massachusetts General Hospital in Boston, called for “changing the culture on how we deal with gallbladder surgery, and particularly the tough gallbladders—to not say you failed because you were not able to take out the gallbladder.” Dr. Lillemoe said surgeons also need to focus on how to prevent mistakes that cause injuries in seemingly less difficult patients. For example, “the real problem out there,” he said, is “the young, postpartum woman who comes in and has a thin, tiny little bile duct and she gets an operation—and her life is destroyed. And those are the easy, low-lying fruit ones that we can eliminate by just teaching the culture of care.”
Part of that culture of care means “we have to put a lot of effort in educating our educators,” Dr. Strasberg said. “We’re graduating residents that don’t know what the critical view of safety is.” If more effort were put into place, he’d be satisfied to see the rates of BDI come down within a few years rather than a generation.
The recommendations will be posted for comment on major surgical society websites, such as SAGES.
Artificial Intelligence May Help Reduce Surgical Errors
Bile duct injuries could be reduced in the near future when surgeons become more trusting of computers to supplement their eyes and training.
Artificial intelligence, now in its early stages in medicine, has already begun to help surgeons; and the more images it sees, the better it will get in identifying tissues, targets and the like. The future of AI-assisted surgery is near.
When a surgeon performing a lap chole is about to make a cut, “the day is not far where your computer will tell you that you are not identifying the critical view of safety,” Dr. Lillemoe said. “And this is not George Jetson talking.” He cited research on bariatric surgery in which computers “can predict when they’re about to make a mistake.”
AI, also known as deep learning, teaches the computer to spot things based on feeding it many thousands of images and associated data. The more images or video (and pixels within the images) the computer sees, the better it gets at identifying problem spots and at adapting algorithms. In addition, computers don’t get tired.
Daniel Hashimoto, MD, MS, the surgical AI and innovation fellow at the same institution, predicted that AI is about three to five years away from being useful in helping with lap chole procedures. He said researchers have used AI to analyze video feeds from an OR in sleeve gastrectomy procedures. The machine examines every frame of the video—24 to 30 per second—and develops “a probability model to predict consequences or what’s going to happen next.” In the sleeve gastrectomy operations, AI’s accuracy rate is at 93% to 94%, Dr. Hashimoto said.
“It’s going to take a lot of data” and effort to determine the right way for computers to assist with surgeries, Dr. Hashimoto said. “It does need a little bit of help from humans.” But, he added, “it’s certainly going to be within our lifetimes when you start to see some aspect of computer assistance.”
However, robots won’t replace surgeons just yet. Dr. Hashimoto was quick to add that “robots aren’t going to take our jobs,” but will “help make smarter decisions.”