Welcome to the January issue of Focus on Fluorescence-Guided Surgery.
In this issue, we have the privilege of interviewing Michael Bouvet, MD, a professor of surgery and the director of endocrine surgery, Division of Surgical Oncology, at the University of California, San Diego. Dr. Bouvet began using fluorescence-guided surgery 20 years ago as a research tool, and is considered one of the pioneers of the technology for endocrine surgery.
We welcome feedback, comments and suggested topics for discussion.
How long have you been using the technology?
Dr. Bouvet: I have been using fluorescence as a research tool in the lab for more than 20 years and as a clinical tool in the OR for the last 10 years.
What is the role of fluorescence-guided surgery (FGS) in endocrine surgery?
Dr. Bouvet: FGS has seen increased interest in recent years. Technological advances have made it more widely accessible for a variety of applications, including thyroid and parathyroid surgery. Parathyroid autofluorescence can be used to help identify parathyroid glands during thyroid or parathyroid surgery and reduce rates of postoperative hypocalcemia after thyroidectomy.1 Fluorescent dyes such as indocyanine green (ICG) may be used to evaluate perfusion of the parathyroid glands during thyroid or parathyroid surgery and help guide decision making about autotransplantation or which gland to leave as a remnant.2 For other endocrine organs, ICG can also be used to assess perfusion of adrenal tumors and pancreatic neuroendocrine tumors.3,4 FGS is an exciting and promising field that may help make endocrine surgery safer, faster and more effective.
What are the procedures for which you find FGS most useful?
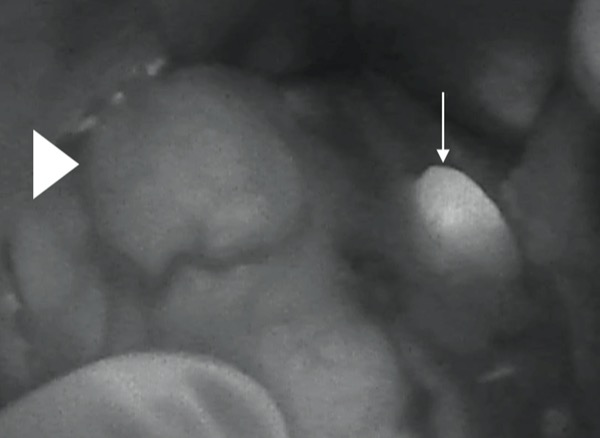
Dr. Bouvet: Autofluorescence is very helpful for identifying normal parathyroid glands during thyroidectomy. Normal parathyroids are very small and can be difficult to identify for even experienced endocrine surgeons. There is an unidentified intrinsic property of parathyroid glands that allows for them to emit a fluorescent signal when excited by near-infrared (NIR) light of the appropriate wavelength. This helps the surgeon to identify normal parathyroids and avoid disruption to their blood supply during thyroidectomy. Both probe- and camera-based systems are now available in the OR to detect parathyroid autofluorescence.
Once the normal parathyroid is identified with autofluorescence (Figure 1 and Video 1), intraoperative mapping angiograms of the parathyroid glands using ICG can be used to protect and preserve the blood supply to the normal parathyroid.5 After the thyroid is removed, ICG can then be used a second time to assess parathyroid gland perfusion.5 Studies from Switzerland have shown that if you have at least one parathyroid gland that is well perfused, as assessed by ICG, postoperative hypocalcemia can be avoided.6
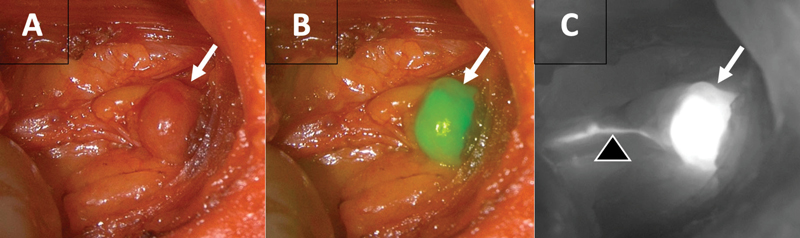
In terms of parathyroidectomy for patients with hyperparathyroidism, ICG can be used to assess the increased perfusion of parathyroid adenomas with commercially available fluorescence imaging systems.7,8 ICG perfusion assessment of parathyroid adenomas can be particularly useful in redo parathyroid surgery where there can be a lot of scar tissue9 (Figure 2 and Video 2). ICG can also be used in patients undergoing subtotal parathyroidectomy for multi-gland disease to ensure there is adequate parathyroid remnant perfusion.10
What are the main benefits for patients?
Dr. Bouvet: Studies have shown NIR fluorescence detection appears helpful for identification and likely preservation of parathyroid glands and that ICG can help assess the perfusion of parathyroid glands. This technology has led to a lower rate of postoperative hypocalcemia for patients undergoing thyroid surgery.
What does a surgeon need to start using this technology?
Dr. Bouvet: While initial studies required customized equipment and software to take advantage of NIR, the increased interest in and demand for NIR intraoperative imaging has resulted in standardized integration into newer models of laparoscopic and robotic imaging systems as well as the development of systems specific to open surgery. As there is no longer a need to use unwieldy and complex systems, the barriers to using this technology have decreased. Fluorescence imaging may now be seamlessly integrated into parathyroid and thyroid operations with the ability to transition instantaneously between fluorescent overlays, gray scale images and traditional white light to allow the surgeon to customize their operation for the safest and most effective operation possible.
Do you believe the technology should be used selectively or routinely?
Dr. Bouvet: I believe the technology should be used routinely in endocrine surgery.
What is the main future of this technology in your field?
Dr. Bouvet: I think we will see advances in the use of fluorescence in endocrine surgery in the near future. For example, fluorescent probes are currently being developed and evaluated for identification of the recurrent laryngeal nerve during thyroid surgery. Identification of the recurrent nerve is critical to reduce inadvertent injury resulting in temporary or permanent hoarseness.
Other advances will include more sensitive and specific fluorescent probes, which are currently being developed in the lab. With fluorescence imaging it is critical to reduce the background signal and maximize the tumor-to-background ratio so that false positives are avoided. There is a tremendous amount of research effort going on now addressing this issue.
What would you recommend for those surgeons who are starting to use the technology?
Dr. Bouvet: I would recommend that surgeons who are interested in the technology first learn about the technique through the multiple webinars and conferences that are available through societies such as the International Society of Fluorescence Guided Surgery, the American Association of Endocrine Surgeons and the American College of Surgeons. In my opinion, it is best to start using this in the routine and straightforward thyroid and parathyroid cases. Surgeons will start to feel more comfortable with the technology and then can apply it to more difficult cases.
Do you have any concluding remarks about the use of fluorescence in endocrine surgery?
Dr. Bouvet: Overall, the use of various fluorescence imaging techniques in endocrine surgery shows promise but requires further investigation. It has been shown to be safe and helpful in several applications, but optimal procedures and uses are only beginning to be defined. Large, well-designed randomized trials with long-term follow-up are needed to determine the utility in preventing permanent hypocalcemia in thyroid surgery and subtotal parathyroidectomy. Quality data regarding operative duration using fluorescence guidance compared with traditional surgery in all fields will also help to define its optimal use and cost-effectiveness, while leveraging artificial intelligence and advances in technology may decrease subjectivity. As FGS becomes more accessible and integrated into imaging platforms, perhaps the barriers to adopting the technology will fall and fluorescence imaging will become even more broadly utilized by endocrine surgeons around the world.
References
- Dip F, Falco J, Verna S, et al. J Am Coll Surg. 2019;228(5):744-751.
- Solorzano CC, Thomas G, Berber E, et al.. Surgery. 2021;169(4):868-878.
- DeLong JC, Chakedis JM, Hosseini A, et al. J Surg Oncol. 2015;112(6):650-653.
- Paiella S, De Pastena M, Landoni L, et al. Surg Endosc. 2017;31(11):4478-4484.
- Benmiloud F, Penaranda G, Chiche L, et al. World J Surg. 2022;46(2):416-424.
- Vidal Fortuny J, Sadowski SM, Belfontali V, et al. Br J Surg. 2018;105(4):350-357.
- DeLong JC, Ward EP, Lwin TM, et al. Surgery. 2018;163(2):388-392.
- Matson J, Lwin TM, Bouvet M. Am J Surg. 2022;223(4):686-693.
- Chakedis JM, Maser C, Brumund KT, et al. BMJ Case Rep. 2015;2015:bcr2015211778.
- Vidal Fortuny J, Guigard S, Diaper J, et al. VideoEndocrinology. 2016;3(1).
- Matson J, Lwin TM, Bouvet M.. Am J Surg. 2022;223(4):686-693.

The International Society for Fluorescence Guided Surgery (ISFGS) is dedicated to the global advancement of FGS, connecting surgeons, nurses, other allied professionals and patients, and growing the overall awareness and implementation of FGS worldwide. Visit ISFGS at www.isfgs.org, and visit the ISFGS patient portal at imageguidedsurgery.net.