Lake Buena Vista, FLA.— A presentation at the 2023 Annual Scientific Assembly of the Eastern Association for the Surgery of Trauma addressed common pitfalls and provided tips for surgeons facing malpractice litigation.
The talk, titled “You’ve Been Served: Survival Skills for Malpractice Litigation,” was part of a panel on Navigating Personal, Clinical, or Career Wrong Turns & Roadblocks. Presenter Matthew Martin, MD, the chief of emergency general surgery at the Los Angeles County + USC Medical Center, shared lessons learned from his experiences as a surgeon and member of a Department of Defense board that reviews malpractice claims.
“Unfortunately, malpractice litigation is something that plagues even the most well-intentioned surgeons,” said panel moderator Tanya Egodage, MD, an assistant professor of surgery at Cooper University Health Care, in Camden, N.J. “Dr. Martin gave the audience knowledge on how to prepare for and deal with this. As some surgeons may not understand the intricacies until they are confronted with litigation, this talk set the framework for preparation in the event that one must deal with it.”
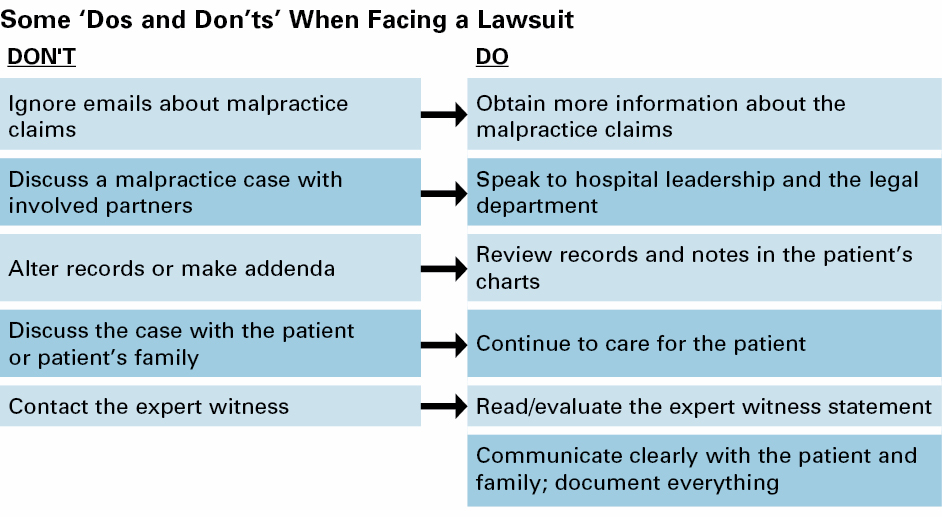
Dr. Martin advised surgeons not to ignore the emails about malpractice claims and take steps to obtain more information about the claim and their role in it. Discuss the case with hospital leadership and the legal department, advised Dr. Martin, but do not discuss the case with any involved partners.
“Seek advice from trusted mentors. A lot of times we don’t talk about this, so you might not know the person in the office next to you went through this horrible experience, too. But when you start asking about it, you’ll find most of us have. Because the odds are if you’re a surgeon, you are going to be involved in at least one of these in your career,” Dr. Martin said.
Dr. Martin recommended reviewing medical records, especially the nursing notes in the patient’s chart, but said to resist the urge to alter records or add addenda. Continue care for the patient if they are still under your care, advised Dr. Martin, but do not talk to the patient or the patient’s family about the case.
If given the option to submit a memo on the case, do so, Dr. Martin said. He advised the audience not to be dismissive or angry in their response, and to instead “write this as if you understand, you know what happened and you understand that there might have been some things that are imperfect. Be objective. Admit any clear errors or problems.”
Dr. Martin also encouraged the audience to utilize and keep any performance improvement/quality improvement or morbidity and mortality review documentation. He noted that having a colleague with experience with malpractice litigation review the memo is critical.
Read and evaluate the expert witness statement, said Dr. Martin, but do not contact the expert witness. Reviewing the expert witness statement can help determine whether the person writing the statement was truly an expert. Dr. Martin noted that many professional societies have standards for expert witness performance and have processes to report transgressions.
| Some ‘Dos and Don’ts’ When Facing a Lawsuit | ||
| DON'T | DO | |
|---|---|---|
| Ignore emails about malpractice claims | Obtain more information about the malpractice claims | |
| Discuss a malpractice case with involved partners | Speak to hospital leadership and the legal department | |
| Alter records or make addenda | Review records and notes in the patient’s charts | |
| Discuss the case with the patient or patient’s family | Continue to care for the patient | |
| Contact the expert witness | Read/evaluate the expert witness statement | |
| Communicate clearly with the patient and family; document everything | ||
“They are often absolutely not an expert. Sometimes they’re in a completely different field, or they’re retired or they’re [in a] nonclinical [role],” Dr. Martin said. “They will make every aspect of the care look like it was malpractice even if it wasn’t. They won’t understand what the legal definition of standard of care is, which is care that would be done by an average provider in your specialty.”
If a case goes to trial, Dr. Martin advised the audience to avoid getting boxed into yes-or-no questions that require more complicated answers, and to never lie, embellish or disparage the patient.
To help avoid malpractice cases, Dr. Martin encourages clear communication with the patient and family, admitting mistakes or errors, and documenting all thought processes.
“If you don’t document your thought process, it didn’t happen. … With every operative report now, I dictate my little blurb at the end, no matter what the resident put. It just says: Here’s what happened, and here’s what we did and here’s why,” Dr. Martin said.
Undergoing a malpractice trial can trigger negative thoughts and emotions and can be a stressful experience for physicians, Dr. Martin noted.
“These can be devastating,” Dr. Martin said. “We’re surgeons, we want to help people; we want to have good outcomes. And then suddenly, you feel like, ‘I’m ashamed of this. My care was bad. I must have done something to generate this case. My partners are going to think less of me; the residents are going to think less of me. I’m going to get fired.’ All of these things hit you.”
Given the impact of these thoughts, Dr. Martin noted the importance of providing support and resources to colleagues involved in malpractice cases.
“Welcome to the team!” Dr. Martin said. “Most of your partners, if they’ve been in surgery long enough, will have gone through something like this. So just reach out and talk to them. You are not the only one who has gone through this.”
“The mere fact that such accomplished surgeons were willing to publicly discuss these relatively taboo issues speaks to the evolution of our specialty,” Dr. Egodage said. “By candidly addressing the difficulties that arise over a surgeon’s lifetime, all of the speakers in this session have given others the knowledge that we encounter many of the same issues, and how to recognize and deal with them appropriately.”