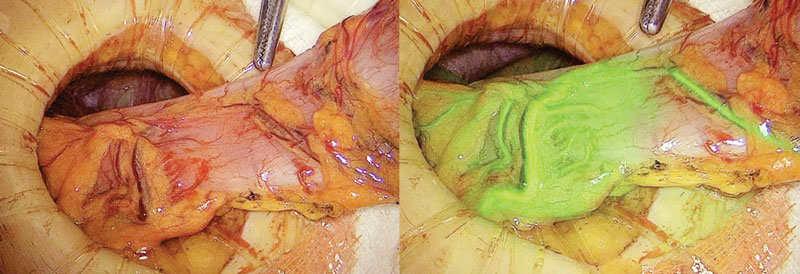
CORAL GABLES, Fla.—As interest in fluorescence-guided surgery (FGS) continues to grow, so does the body of research supporting the use of fluorescence-guided perfusion assessment to reduce the risk for anastomotic leaks, said Steven D. Wexner, MD, PhD (Hon), at the 2023 annual meeting of the International Society for Fluorescence Guided Surgery.
“Virtually every study since the PILLAR II trial has shown significant potential benefit to ICG [indocyanine green] as it seems to be associated with very low levels of anastomotic leak even in high-risk anastomoses,” Dr. Wexner, the director of the Ellen Leifer Shulman and Steven Shulman Digestive Disease Center and chair of the Department of Colorectal Surgery at Cleveland Clinic in Weston, Fla., told General Surgery News.
“Whether those studies are from North America, Asia, Europe or the United Kingdom, they all show the same findings,” he added.
Establishing some context, Dr. Wexner said the estimated rate of anastomotic leaks for high-risk anastomoses is between 10% and 15%. But in the PILLAR II trials, in which Dr. Wexner and his colleagues from 11 U.S. centers used ICG to assess perfusion in 139 patients undergoing left-sided colectomy and anterior resection, the anastomotic leak rate was less than 2% (J Am Coll Surg 2015;220[1]:82-92).
These findings were confirmed by a larger multicenter trial analyzing the use of ICG and near-infrared (NIR) imaging in 504 patients undergoing elective colorectal operations at centers in Switzerland, the United Kingdom and Ireland. The anastomotic leak rate was again far below typical estimates, at 2.4% overall. Use of NIR-ICG assessment also had an impact on intraoperative decision making—surgeons in this trial changed the site of bowel division in 29 patients (5.8%), who subsequently did not experience leaks (Br J Surg 2018;105[10]:1359-1367).
Although both those trials involved laparoscopic procedures, a trial of sphincter-saving surgery in 436 rectal cancer patients undergoing curative operations found that ICG imaging also reduced the risk for anastomotic leak in robotic-assisted procedures. The anastomotic leak rate in the 123 patients who had ICG imaging was 0.8%, compared with 5.4% in the 313 patients who did not have such imaging (P=0.031) (Int J Med Robot 2016;12[4]:710-717).
“The rate of anastomotic leak was almost a magnitude less, and subsequent studies showed ICG imaging could be used in a variety of settings,” Dr. Wexner said.
A systematic review and meta-analysis of five studies involving more than 1,302 patients found that intraoperative ICG fluorescence imaging significantly reduced the rate of anastomotic leaks in colorectal surgery compared with standard care (Tech Coloproctol 2018;22[1]:15-23). “That shows that with a bit more data, there is clearly a benefit, but this study does not include publications from the last seven years,” Dr. Wexner said.
The growing evidence overwhelmingly supports the use of ICG fluorescence to reduce the rate of anastomotic leaks, but there has been one outlier, which found no difference in anastomotic leak rate between ICG imaging and standard care (Dis Colon Rectum 2021;64[8]:995-1002). “That study, unfortunately, was prematurely terminated and never fulfilled the required enrollment to achieve statistical significance. Even though they have statistics, they’re not valid,” Dr. Wexner said. The study had planned to recruit up to 800 patients over two years but ended up with only 347.
But if the number of studies of FGS is any indication—an entire recent issue of the journal Surgery was devoted to the topic of fluorescence imaging—researchers are piqued by its potential. Included in that issue was a Delphi survey of 35 international experts who, after only two rounds, found a 70% consensus on 60 of 69 statements (Surgery 2022;172[6S]:S38-S45). “There is a lot of interest and a lot of benefit,” Dr. Wexner said.
Dr. Wexner is a paid consultant for Intuitive Surgical, Medtronic, Olympus and Stryker, and receives royalties for intellectual property license from Intuitive and Karl Storz.