|  |  |
AVENTURA, Fla.—Lymphatic leakage after inguinal hernia repair is a rare but known occurrence. In a recent case that warranted surgical exploration, the novel use of indocyanine green (ICG) lymphangiography helped the surgical team not only identify the leak but also successfully repair it.
The case, likely the first of its kind reported in the literature, involved a 74-year-old woman who had undergone open inguinal hernia repair with mesh and a plug to manage a recurrent incarcerated left inguinal hernia.
“Over the next two weeks during her follow-up visits, she was noted to have a fluid collection in her left inguinal area,” said Samuel Szomstein, MD, the associate director of the Bariatric and Metabolic Institute and Division of Minimally Invasive Surgery, and director of Fellowship in Advanced MIS and Bariatrics at Cleveland Clinic in Weston, Fla., who presented the case at the 2024 meeting of the International Society for Fluorescence Guided Surgery.
At the outpatient clinic, Dr. Szomstein drained the fluid, about 200 mL of a milky substance, on two separate occasions, but both times the swelling recurred within a few days. CT imaging revealed a large fluid collection consistent with a suspected diagnosis of lymphatic leakage. Soon after, the patient was taken to surgery.
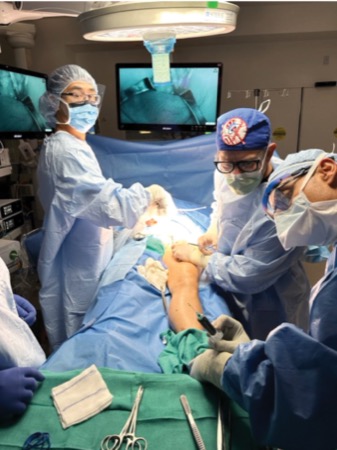
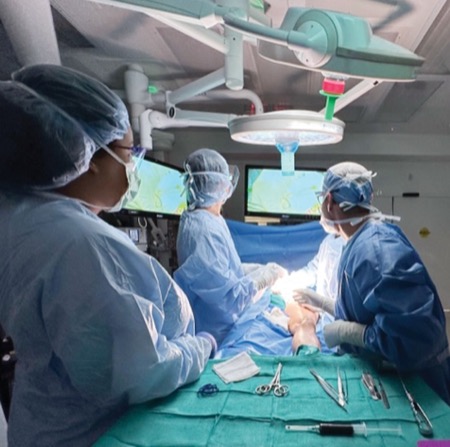
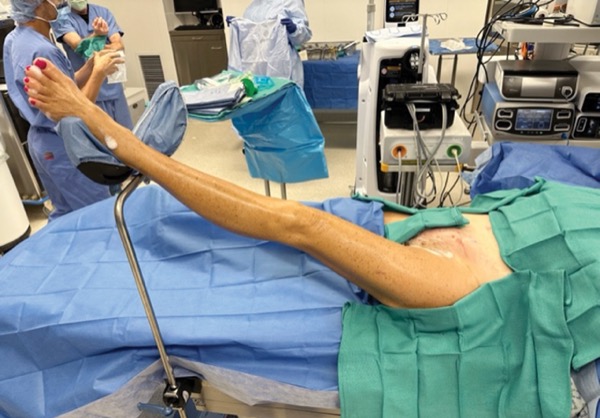
After opening the skin at the previous incision site, the surgical team dissected down until they encountered fluid after opening the external oblique. They then injected ICG into the first web space between the patient’s big and second toes and massaged the leg to encourage drainage of the lymphatics toward the inguinal lymph nodes.
The team used a Spy portable handheld imaging system (Stryker) using near-infrared imaging to visualize the lymphatics. In Spy fluorescence mode, the lymphatics appeared white, tracking up the leg. “We toggled between Spy fluorescence mode and overlay mode for improved visualization of the lymphatic leaks,” Dr. Szomstein said, noting that they had to remove the mesh to be able to properly evaluate and identify the area of leakage.
In overlay mode, the lymphatics and ICG showed as green superimposed on a background of normal white light. The area of the leak appeared to be on the sidewall of the lymphatic vessel, so the suture repaired it; they also clipped the ends of some lymphatic tributaries.
To the naked eye, the leak appeared closed, but further evaluation with ICG showed continued leakage. “As such, we continued the dissection and mobilization until we found a leak of the lymphatic vessels deeper. This was then carefully closed,” Dr. Szomstein said.
When reexamination of the area showed resolution of the lymphatic leakage and no further visible leaks, the team reattached the mesh and repaired the hernia. The patient recovered well and has not had a recurrence of lymphatic leakage.
“This was a very interesting case in which ICG proved to be a valuable adjunct to surgical management,” Dr. Szomstein said.
AVENTURA, Fla.—Lymphatic leakage after inguinal hernia repair is a rare but known occurrence. In a recent case that warranted surgical exploration, the novel use of indocyanine green (ICG) lymphangiography helped the surgical team not only identify the leak but also successfully repair it.
The case, likely the first of its kind reported in the literature, involved a 74-year-old woman who had undergone open inguinal hernia repair with mesh and a plug to manage a recurrent incarcerated left inguinal hernia.
“Over the next two weeks during her follow-up visits, she was noted to have a fluid collection in her left inguinal area,” said Samuel Szomstein, MD, the associate director of the Bariatric and Metabolic Institute and Division of Minimally Invasive Surgery, and director of Fellowship in Advanced MIS and Bariatrics at Cleveland Clinic in Weston, Fla., who presented the case at the 2024 meeting of the International Society for Fluorescence Guided Surgery.
At the outpatient clinic, Dr. Szomstein drained the fluid, about 200 mL of a milky substance, on two separate occasions, but both times the swelling recurred within a few days. CT imaging revealed a large fluid collection consistent with a suspected diagnosis of lymphatic leakage. Soon after, the patient was taken to surgery.
After opening the skin at the previous incision site, the surgical team dissected down until they encountered fluid after opening the external oblique. They then injected ICG into the first web space between the patient’s big and second toes and massaged the leg to encourage drainage of the lymphatics toward the inguinal lymph nodes.
The team used a Spy portable handheld imaging system (Stryker) using near-infrared imaging to visualize the lymphatics. In Spy fluorescence mode, the lymphatics appeared white, tracking up the leg. “We toggled between Spy fluorescence mode and overlay mode for improved visualization of the lymphatic leaks,” Dr. Szomstein said, noting that they had to remove the mesh to be able to properly evaluate and identify the area of leakage.
In overlay mode, the lymphatics and ICG showed as green superimposed on a background of normal white light. The area of the leak appeared to be on the sidewall of the lymphatic vessel, so the suture repaired it; they also clipped the ends of some lymphatic tributaries.
To the naked eye, the leak appeared closed, but further evaluation with ICG showed continued leakage. “As such, we continued the dissection and mobilization until we found a leak of the lymphatic vessels deeper. This was then carefully closed,” Dr. Szomstein said.
When reexamination of the area showed resolution of the lymphatic leakage and no further visible leaks, the team reattached the mesh and repaired the hernia. The patient recovered well and has not had a recurrence of lymphatic leakage.
“This was a very interesting case in which ICG proved to be a valuable adjunct to surgical management,” Dr. Szomstein said.
“If we had not used ICG to show the repair was unsuccessful, we would have stopped after the initial attempt of repair and clipping, thinking we had accomplished our objective.”