By Monica Smith
BOSTON—The year 2022 saw all-time records set for organ transplantation, but significant gaps remain. At last year’s Clinical Congress of the American College of Surgeons, transplant surgeons discussed strategies for expanding programs and increasing the number of lifesaving transplants.
In the mid-2010s, the kidney transplant program at NYU Langone Health picked up significantly, from about 30 kidneys per year in 2016 to 157 the following year. When Zoe Stewart Lewis, MD, PhD, MPH, came on board in 2018, the division launched a pediatric program and a program for transplanting hepatitis C virus−positive organs into uninfected patients.
“The numbers that year were stable” at 175, Dr. Stewart Lewis said, “but it was a very different type of transplanting”-that is, they began employing strategies that allowed them to import more organs. In 2021, NYU Langone became the first hospital to surpass 300 kidney transplants in New York City, without sacrificing good patient outcomes.
“It starts with giving every potential organ offer a chance: rather than, ‘Is this a good kidney?’ asking ‘Who is the right recipient for this kidney?’” said Dr. Stewart Lewis, now the director of the Transplant Institute at University Hospitals, in Cleveland. About one-third of patients fall off the waitlist because they become too sick or die, so waiting until the perfect kidney becomes available may not be the best strategy, she said. “Transplanting patients in the 60-plus age group is where we have the opportunity to help more patients.”
Donor After Cardiac Death Organs
One programmatic strategy to increase the pool of usable organs is a willingness to use donor after cardiac death (DCD) organs. “There continues to be a strong reluctance to use DCD kidneys from donors over 50, which I think is a disservice to patients. The majority of these kidneys will work perfectly fine when properly screened,” Dr. Stewart Lewis said.
Another approach is to expand acceptable ischemic cold times. “We routinely transplant organs at 36 to 45 hours,” she said, noting some important considerations: You need a strong cross-matching program and a willingness to get creative with travel logistics. “I drove a kidney from Iowa 14 hours to get to Cleveland because I couldn’t get a flight,” Dr. Stewart Lewis said.
The group also works with surgically damaged kidneys after reconstructing them, and with kidneys that have multiple arteries. “Does anyone want to do a dual organ transplant? Not really, but your patients can do well and have great outcomes,” she said.
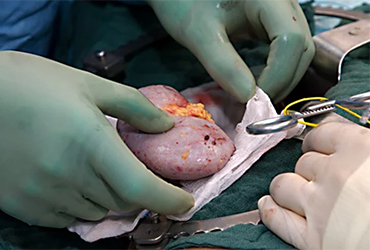
Since moving to Case Western, Dr. Stewart Lewis has been able to apply similar tactics to boost volume while maintaining good outcomes, and said if she had a bumper sticker on her car, it would read “Give Every Organ a Chance.”
“It’s easy to find the ‘no’ in an organ offer. We may have to push ourselves at times to find a ‘yes,’ and to think about how to make this the right organ for the right patient on the list,” she said.
DCD in Liver Transplantation
Procurement of DCD organs is a strategy also used in liver transplantation by Amit K. Mathur, MD, a professor of surgery at Mayo Clinic in Scottsdale, Ariz., and his colleagues. Although this tactic has increased fourfold in the past decade, it still represents only 10% of liver transplants in the United States, while making up 20% to 50% of the volume in some European countries, Dr. Mathur said. “There’s a huge opportunity for U.S. programs to use DCD liver transplants.”
Dr. Mathur speculated that the reluctance to do so is fear of poor outcomes based on early reports. His own program experienced two major classes of complications when they started using DCD livers: early allograft dysfunction and ischemic cholangiopathy.
“It was clear from the literature and our own practice that ischemic cold preservation was driving post-transplant complications and outcomes. If we wanted to grow DCD transplants, we needed to change the game,” Dr. Mathur said.
There are some novel strategies available for those who want to expand their liver transplant program using DCD organs. They are normothermic perfusion (NMP), for which there are two FDA-approved devices (TransMedics Organ Care System and OrganOx metra), normothermic regional perfusion (NRP) and hypothermic perfusion.
“Our focus has been on the first two. In comparison studies, early allograft dysfunction in NMP and NRP is relatively comparable, as are the grafts’ viability,” Dr. Mathur said, noting that a recent small study showed both approaches were superior to cold storage DCD, with NRP having the best biliary outcome.
Besides outcomes, a major difference between NMP and NRP is cost, said Jordan Hoffman, MD, a thoracic and cardiac surgeon and an associate professor of surgery at the University of Colorado School of Medicine, in Aurora.
“TransMedics is a $60,000 to $80,000 device depending on your contract with the company, compared with less than $5,000 for NRP. TransMedics is one organ per device while NRP perfuses the entire donor, up to eight organs,” Dr.Mathur said. These differences mean a much lower cost per organ with NRP. “Depending on an institution’s equipment and personnel, we’ve demonstrated that we can perform more than 20 organ recoveries with the TA-NRP technology for every one ex situ machine perfusion.”
Dr. Mathur’s program uses the TransMedics Organ Care System for several reasons, one being portability—it fits on an airplane, allowing procurement from across the country. Since his program started using the device in 2022, DCD livers have become the majority of liver transplants, making up 62%. The ease of clinical logistical arrangements in donor and recipient OR times has allowed them to travel much farther to procure organs, he said. “We’ve been able to go nearly 2,000 nautical miles to procure livers for patients by using these devices.”
Overall, Dr. Mathur believes that NMP solves many problems: The number of DCD donors means increased organ availability, so they’re able to list more patients who get transplanted faster and have excellent survival rates. “We are restoring the quality of donor organs and that will translate into Scientific Registry of Transplant Recipients outcomes as well,” he said, but he acknowledged that cost remains a concern.
“Perfusion is an expensive endeavor in the NMP space, more so than in the NRP space, so that’s something our institution continues to tackle,” Dr. Mathur noted.
