SAN FRANCISCO—When the American College of Surgeons held its annual Clinical Congress last October, one of the meeting’s most popular sessions once again proved to be “10 Hot Topics in General Surgery,” a fast-paced roundup of the practice’s most exciting innovations and developments. Here we summarize the first five presentations from that session.
Use of Ultrasound in the Diagnosis of Inguinal Hernia
Benjamin K. Poulose, MD, MPH, the Robert M. Zollinger Lecrone-Baxter Chair and chief of general and gastrointestinal surgery at The Ohio State University Wexner Medical Center, in Columbus, kicked off the session by discussing the diagnosis and management of inguinofemoral hernia using ultrasound.
“The larger context of this discussion is there are limits to all modalities of inguinofemoral hernia diagnosis, which really comprises history and physical exam, ultrasound, CT, and MR,” he began. “On occasion, you may not come to a definitive diagnosis with the initial patient visit, and that’s OK.”
A 2020 article provided a comprehensive summary of the different diagnostic modalities in inguinal hernia (Hernia 2020;24[5]:917-926). The authors found that ultrasound has higher sensitivity and specificity than either CT or MRI, although its performance is dependent on the operator’s level of expertise.
Dr. Poulose then offered a practical approach for diagnosing patients, one he said begins with a history and physical exam. If those suggest an inguinofemoral hernia, patients can be offered an operation. If the history does not indicate inguinofemoral hernia but one is found on physical exam (typically in an asymptomatic patient), either an operation or watchful waiting can be offered.
Things get more complicated when the history suggests a hernia but the physical exam does not concur. In this case, patients can be offered an operation with a caveat, imaging or watchful waiting. Finally, when both history and physical exam are not suggestive of a classic inguinofemoral hernia, clinicians should consider imaging or another diagnosis.
In patients with a positive history and negative physical exam, an operation with a caveat suggests several potential therapeutic approaches. Surgeons performing a transabdominal preperitoneal approach should not rely on the intraperitoneal view since preperitoneal fat can obscure the defect. Dr. Poulose also suggested exploring both the inguinal and femoral spaces. “But this is still not as great a result as if you detected a hernia on physical examination,” he said.
Imaging is a good adjunct in these circumstances, whereas ultrasound can help identify the hernia; CT works well in patients with large body habitus, and MRI is important when core muscle injuries, for example, are suspected. Watchful waiting may see the patient return for follow-up, when aggravating factors can be addressed; physical therapy is also an option. It’s more challenging when the history and physical exam are both negative. Imaging plays a role here: Another diagnosis should be considered, particularly if a mass is present.
Despite the important role ultrasound plays, Dr. Poulose admitted there are difficulties with its use. It is very user dependent; the radiologist is decoupled from the ultrasound tech, removing the real-time ability to fine-tune the ultrasound study; body habitus can be confounding; and there are inherent challenges in trying to image a 3D area with 2D imaging.
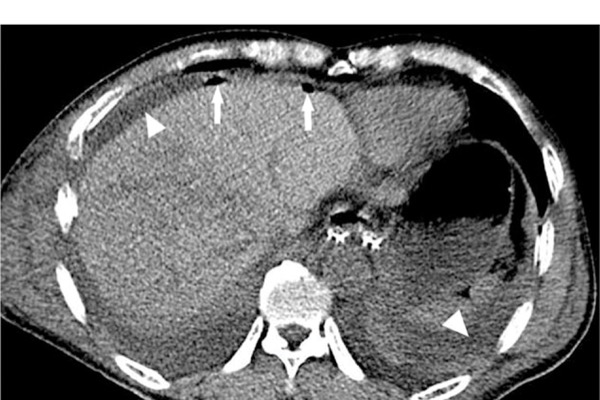
Anastomotic Failure in Blunt Abdominal Trauma
Sharmila Dissanaike, MD, the chair of surgery at the University of New Mexico, in Albuquerque, discussed hollow viscus injuries and how often they occur in blunt trauma, whether delaying diagnosis worsens such injuries, and what makes such injuries more likely to leak.
As Dr. Dissanaike explained, as many as 6% of blunt trauma injuries are hollow vicsus injuries. Although penetrating injuries are usually full-thickness injuries, the more common blunt trauma injuries are often either from ischemia or a partial-thickness injury, both of which present at a later time. “Delayed diagnosis, delayed presentation and, as a result, delayed treatment are a very common problem in this particular diagnosis,” she said.
Does this delay worsen outcome? Of note, a 2018 systematic review found no difference in delayed-intervention patients compared with those who were diagnosed sooner (Eur J Trauma Emerg Surg 2018;44[3]:369-376). “So, to date, we don’t have proof that the delay actually harms patients,” she said.
Does small intestine versus colon matter? This question was examined in a multicenter series of nearly 1,000 injuries. The study found that the adjusted risk ratio for anastomotic leak was more than double in the colon (4.83) than in the small intestine (2.32). Anastomotic leak also was found to result in increased infections, ventilator days, ICU length of stay, total LOS, reoperation and readmission rates (Am J Surg 2023;226[6]:770-775).
In that study, the researchers examined a sub-cohort of patients with bucket-handle injuries. Here it was found that anastomotic leak occurred in 5.2% of such patients, compared with 1.2% for those who did not have bucket-handle injuries. The study found that surgical technique did not affect leak rate, although a number of other factors did: blood transfusion, patient illness or illness severity, increased comorbid conditions, and, to a much smaller degree, male sex.
That study also found that after correcting for a number of other potentially confounding factors such as comorbidities and injury severity, one that was associated with increased anastomotic leak was whether the initial operation was damage control surgery.
“If the belly was left open, it doubled the risk of anastomotic leak,” Dr. Dissanaike said. “So maybe we’re damage-controlling a little bit too much.”
Clinical Approach to Transgender Patients With a Breast Mass
Diane M. Krutzler-Berry, MD, an assistant professor of surgery at Marshall Health in Barboursville, W.Va., discussed the influence of gender-affirming surgery and hormone therapy on breast cancer, diagnostic considerations in transgender populations, and physical and psychological factors to be considered in breast cancer diagnoses.
“There are 1.4 million people who identify as transgender in the United States today, which has doubled over the last decade and will likely continue to grow,” Dr. Krutzler-Berry began. Among these people, gender-affirming surgery includes procedures such as mastectomy (top surgery) and genital surgery. And while both feminizing and masculinizing hormone therapy can also influence breast cancer risk in these individuals, psychological and social factors can act as barriers to screening.
Breast cancer screening (an annual mammography) in transgender women should begin at approximately 50 years of age and after five years of exogenous hormone use. Such procedures are gender-affirming, thereby increasing their level of importance for transgender women. In transgender men who have not undergone top surgery, screening should begin at age 40, unless a family history indicates an earlier start. Cancer risk still exists in transgender men who have undergone gender-affirming surgery, necessitating a physical exam of the chest wall and axilla beginning at age 50.
With respect to risk reduction, top surgery reduces breast cancer risk by up to 90%. Nevertheless, high-risk patients still need a preoperative workup, including a family history, genetic testing and breast MRI. In a 2018 meta-analysis of male-to-female transgender patients, researchers found that the median age for breast cancer diagnosis was significantly earlier in transgender men (51.5 years) than in either cisgender men (68 years) or cisgender women (60 years) (Eur J Surg Oncol 2018;44[10]:1455-1462).
In perhaps the most well-known study on the subject, researchers found that the rate of breast cancer was 46 times greater in transgender women than cisgender men (BMJ 2019;365:l1652). That investigation also found that four of 1,229 transgender men developed breast cancer, a rate Dr. Krutzler-Berry said was lower than expected.
Treatment of these individuals follows gold-standard therapies for cisgender patients. Nevertheless, the choice to continue or discontinue hormone therapy needs to be made on an individual basis.
“You really need to involve a multidisciplinary group, with the cancer team, psychology and endocrinology to treat these patients appropriately and manage their hormone therapy while they’re going through breast cancer treatment,” Dr. Krutzler-Berry added. “And remember, there is a psychological impact to stopping these hormones, so don’t take this lightly when you are dealing with this population.”
Management of the Axilla After Neoadjuvant Therapy For Breast Cancer
Rachel L. McCaffrey, MD, an assistant professor of surgery at Vanderbilt University Medical Center, in Nashville, Tenn., tackled the topic of axilla management in node-positive patients who convert to node-negative status after completing chemotherapy.
“The current literature states that targeted dissection or sentinel lymph node biopsy, with certain caveats, is adequate in this population,” she said. “But you have to figure out which patients fit in that scenario.”
The first step is determining the burden of nodal disease through physical exam and imaging. Patients with large, bulky nodes are less likely to convert to cN0. Clinicians also need to consider the cancer subtype, where HER2-positive and triple-negative disease are much more likely to have a pathologic complete response than hormone-positive disease.
After completion of chemotherapy, both the physical exam and imaging should be repeated. Whether this comprises ultrasound, MRI or both is dependent on institutional factors. Patients who are still clinically node-positive after chemotherapy will require an axillary dissection. If the patient is clinically node-negative, surgeons should consider targeted dissection or sentinel lymph node biopsy, provided three lymph nodes are removed, dual tracer is used and the clipped node is removed. Finally, the possibility for intraoperative analysis should be discussed with the patient.
Outcomes after targeted dissection or sentinel lymph node biopsy can result in either a pathologic complete response or pathologic node-positive disease. In pathologic complete response, radiation is still recommended. If node-positive disease persists, reoperation for axillary dissection is a reality, with consideration of lymphovenous bypass.
“There’s controversy if lymphovenous bypass actually improves anything in the prophylactic space,” Dr. McCaffrey explained. “But if the patient’s already under anesthesia for a couple hours, is one additional hour of anesthesia for possible prevention of life-altering lymphedema worth it? Probably yes.”
Endoscopic Retrograde Treatment For Appendicitis: Real or Not?
Steven D. Wexner, MD, PhD, the director of the Ellen Leifer Shulman and Steven Shulman Digestive Disease Center at Cleveland Clinic Florida, in Weston, discussed endoscopic appendicitis treatment.
“I last took out an appendix in isolation in 1986 or 1987,” Dr Wexner began. “But I take them out almost daily as appended to the cecum as part of some type of colectomy.”
According to Dr. Wexner, the endoscopic retrograde appendicitis treatment (ERAT) was first described in 2012, a process that comprises colonoscopy followed by retrograde endoscopic cholangiopancreatography of the appendix (Gastrointest Endosc 2012;76[4]:862-866).
“That means getting into the appendiceal orifice, injecting contrast to find the foreign material, irrigating it and, in some cases, putting a stent in the appendiceal lumen to prevent recurrence,” he said.
To date, most relevant studies on the subject have been performed in China, including a recent effort of 110 patients. In that trial, ERAT patients had outcomes comparable to those who underwent traditional appendectomy, except ERAT patients had a three-year recurrence rate of 14.5% (J Dig Dis 2022;23[11]:636-641).
By 2023, a meta-analysis on the subject had examined 2,236 cases and controls from 26 randomized controlled trials (Clin Res Hepatol Gastroenterol 2023;47[10]:102241). The analysis found a number of benefits in ERAT patients, including shorter procedure time, LOS and bed rest, plus a lower incidence of complications and quicker return to normal temperature. The only drawback to the technique was a higher recurrence rate.
The technique has evolved further to a single-use SpyGlass (Boston Scientific) technique offering a direct view of the appendiceal lumen, which was examined in a 2024 study with encouraging results (Surg Endosc 2024;38[10]:6156-6160).
“But after reviewing all of these articles, I’ve got to say the jury is still out in my mind,” Dr. Wexner concluded.
Dr. Poulose reported consulting fees from Ethicon; equity holdings with EndoEvolve LLC; research support from Advanced Medical Solutions and Bard-Davol; and salary support from the Abdominal Core Health Quality Collaborative. Dr. Dissanaike reported a financial relationship with Heron Therapeutics.