
Abdominal Infection and Sepsis in Immunocompromised ICU Patients
Paiva JA, Rello J, Eckmann C, et al. Abdominal Sepsis Study (AbSeS) group for the Trials Group of the European Society of Intensive Care Medicine. Intra-abdominal infection and sepsis in immunocompromised intensive care unit patients: disease expression, microbial aetiology, and clinical outcomes. Eur J Intern Med. 2024;129(7):100-110. doi:10.1016/j.ejim.2024.07.019
Summary: Secondary analysis of the prospective “AbSeS” database (309 ICUs, 42 countries) compared the epidemiology of intraabdominal infection (IAI) between immunocompromised (IC) and non-IC ICU patients and to identify risk factors for mortality. Immunocompromised was defined as neutropenia, “prolonged” glucocorticoid use, prior chemotherapy or radiotherapy (within one year), bone marrow or solid-organ transplantation, congenital, or other immunosuppressive drug use. Mortality was defined in the ICU at any time, or 28-day mortality for those discharged earlier. Among 2,589 patients, 239 (9.2%) were IC, most with secondary peritonitis. IAIs were mostly hospital-associated; typhlitis was more common, whereas biliary infections were less common. There were no differences in disease severity (except shock was more frequent with IC), in pathogens, resistance patterns, or organ dysfunction. Mortality was similar between groups (31% vs. 29%; IC vs. non-IC, respectively; odds ratio [OR], 0.98; 95% CI, 0.66-1.43). By logistic regression, independent risk factors for mortality among IC patients included septic shock at presentation (OR, 6.64; 95% CI, 1.27-55.72) and unsuccessful source control (OR, 5.48; 95% CI, 2.29-12.57).
Commentary: Everybody worries about IC patients. Dogma holds that, even as we struggle to define exactly what IC is, such patients are at high risk for adverse outcomes. These data suggest not. Unfortunately, despite this report, a consensus definition remains elusive. (Note that diabetes mellitus was not considered). Perhaps a new, useful biomarker will be identified in the future. The mortality rate of about 30% is consistent with several other reports of IAI requiring ICU care. The bottom line: Provided shock is reversed expeditiously and source control is obtained in a timely manner, IC patients with IAI are the same as their “competent” brethren. Treat them the same, including antibiotic management, and expect similar outcomes.
Povidone-Iodine or Chlorhexidine for Preoperative Skin Antisepsis?
Widmer AF, Atkinson A, Kuster SP, et al. Povidone iodine vs. chlorhexidine gluconate in alcohol for preoperative skin antisepsis: a randomized clinical trial. JAMA. 2024;332(7):541-549. doi:10.1001/jama.2024.8531
PREP-IT Investigators. Skin antisepsis before surgical fixation of extremity fractures. N Engl J Med. 2024;390(5):409-420. doi:10.1056/NEJMoa2307679
Summaries: Widmer et al enrolled 3,360 patients (three Swiss tertiary hospitals; cardiac [n=2,187 (65%)]; abdominal [n=1,173 (35%)]) to compare povidone-iodine in alcohol (PVIa) with chlorhexidine gluconate in alcohol (CGa) to prevent surgical site infection (SSI) after cardiac or abdominal surgery in a cluster-randomized, crossover noninferiority trial. Sites were randomly assigned monthly (26 cluster periods) to either use PVIa or CGa according to a standardized protocol. Primary outcome was SSI within 30 days (for abdominal operations) or one year (cardiac) using standard CDC definitions. The noninferiority margin was 2.5%. Secondary outcomes included SSIs stratified by infection depth and type of surgery. In all, 1,598 patients were assigned to PVIa vs. 1,762 patients who received CGa. There were no differences in age (mean, 65 years) or sex (mean, 33.5% female). Incidences of SSI (5.1% for PVIa; 5.5% for CGa; difference, 0.4% [95% CI, –1.1% to 2.0%]) did not exceed the predefined noninferiority margin before or after correction for clustering. The unadjusted relative risk (RR) for PVIa vs. CGa was 0.92 (95% CI, 0.69-1.23). After cardiac surgery, SSI rates were 4.2% for PVIa and 3.3% for CGa (RR, 1.26; 95% CI, 0.82-1.94), whereas after abdominal surgery, SSI rates were 6.8% for PVIa and 9.9% for CGa (RR, 0.69; 95% CI, 0.46-1.02).
The PREP-IT investigators conducted a cluster-randomized, crossover trial at 25 U.S. and Canadian hospitals to use 0.7% iodine povacrylex (PVX) in 74% isopropyl alcohol or CGa as preoperative antisepsis for surgical repair of extremity fractures. Every two months, hospitals alternated interventions. Separate populations of patients with open fractures (OFs, n=1,700) or closed fractures (CFs, n=6,875) were sub-analyzed. The primary outcome was SSI (superficial within 30 days, or deep or organ-space infection within 90 days). The secondary outcome was unplanned reoperation for fracture-healing complications. After CF repair, SSI incidence was 2.4% after PVX vs. 3.3% after CGa (OR, 0.74; 95% CI, 0.55-1.00; P=0.049). In the OF population, SSI incidence was 6.5% after PVX vs. 7.3% after CGa (OR, 0.86; 95% CI, 0.58-1.27; P=0.45). Frequencies of unplanned reoperation, serious adverse events, and one-year outcomes did not differ.
Commentary: Preoperative skin antisepsis is integral to SSI prevention. A landmark 2010 report showed CGa to be superior to PVI (without alcohol) for SSI prevention after clean-contaminated operations (Darouiche et al, doi:10.1056/NEJMoa0810988). Time has shown that alcohol is probably the crucial component for SSI prevention. Here, in the first study, PVIa was noninferior to CGa for prevention of SSI after cardiac or abdominal surgery. In the second study, PVX was superior to CGa for SSI prevention, but only for CFs. Are there meaningful differences between these reports, besides the obvious (the types of operation studied)? The sample size in the OF group was much smaller (although not inherently smaller), so the possibility of underpowering exists, but is mitigated by the higher incidence of SSI after OFs. Is the concentration of isopropyl alcohol crucial (74% for PVX and 70% for the other agents)? Or, is PVX inherently different from PVIa apart from the alcohol concentration?
Morbidity and Mortality of Surgery for Perforated Gastroduodenal Ulcer
Abouelazayem M, Jain R, Wilson MSJ, et al. Global 30-day morbidity and mortality of surgery for perforated peptic ulcer: GRACE study. Surg Endosc. 2024;38(8):4402-4414. doi:10.1007/s00464-024-10881-0
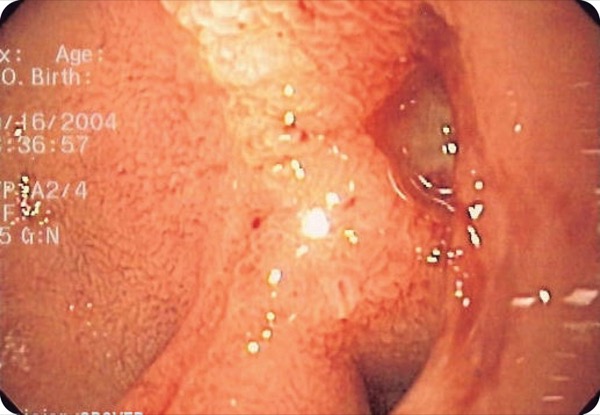
Summary: This study evaluated characteristics and global 30-day morbidity and mortality of patients undergoing surgery for gastroduodenal ulcer perforation (GDUP) and to identify parameters associated with outcomes. There were 1,874 adult patients (159 centers, 52 countries) who underwent GDUP surgery in the first six months of 2022. Patients with gastric cancer were excluded.
Patients were stratified by age (±50 years) and time from symptom onset to presentation (=24 hours). Patients were 78% male; median age was 49 years. 30-day morbidity and mortality were 49% and 9%, respectively. Median hospital stay was seven days. Open surgery was performed in 80% of cases. Risk factors for mortality included age >50 years (OR, 4.7; 95% CI, 3.1-7.6), female gender (OR, 1.9; 95% CI, 1.3-2.9), shock on admission (OR, 4.8; 95% CI, 3.2-7.1), and acute kidney injury (OR, 3.9; 95% CI, 2.7-5.6). Delayed presentation was associated with 30-day morbidity (OR, 1.3; 95% CI, 1.1-1.6) but not mortality.
Commentary: In the West, we tend to forget about GDUP in this era of effective, ubiquitous oral gastric acid reduction therapy and (overused) parenteral prophylaxis of critically ill patients. Cases are encountered seldomly, laparoscopic repair predominates, operative mortality is <5%, and most patients require only antimicrobial prophylaxis because peritonitis is chemical from acid injury initially, with bacterial infection a secondary phenomenon. This is a reminder that GDUP is a major global health problem. Unfortunately, little information is provided regarding preoperative morbidity (ulcer symptoms or therapy) or antibiotic management.
Timeliness of Operation in Emergency General Surgery
Silver DS, Lu L, Beiriger J, et al. Association between timing of operative interventions and mortality in emergency general surgery. Trauma Surg Acute Care Open. 2024;9(1):e001479. doi:10.1136/tsaco-2024-001479
Summary: This retrospective study explored relationships between hospital arrival-to-operation time (tOR) and in-hospital mortality in emergency general surgery (EGS). Four hospitals enrolled adults who underwent surgery for a primary American Association for the Surgery of Trauma–defined EGS diagnosis between 2021 and 2023. Patients undergoing surgery more than 72 hours after admission were excluded as nonurgent. tOR was defined as time from initial capture of vital signs to skin incision. A mixed-effect hierarchical multivariable model for mortality adjusted for demographics, comorbidities, organ dysfunction, and hospital-level clustering. In all, 1,199 patients were included. Median tOR was 8.2 hours (IQR, 5-21 hours). Prolonged tOR increased the odds of mortality. Patients undergoing surgery between 6.7-10.7 hours and 24.4-70.9 hours had the highest (comparable) risk-adjusted odds of mortality compared with those having surgery in less than 4.2 hours after admission (reference quintile) (adjusted OR [aOR], 68.99; 95% CI, 4.61-1,032.98; P=0.002; aOR, 69.68; 95% CI, 2.97-1,636.04; P=0.008).
Commentary: Timely intervention is an argument to provide EGS services, yet data regarding triage and timing are limited. Prompt EGS intervention was associated with lower in-hospital mortality. The observation is partially concordant with Surgical Infection Society updated guidelines (Huston et al, doi:10.1089/sur.2024.137) for complicated IAI management, which recommend surgical intervention within 12 hours (six hours for patients with shock). These results can inform triage and intervention in the EGS population, but beware the wide confidence intervals that reflect the small sample and heterogeneity of included conditions. Exclusion of perforated appendicitis is both a strength and weakness, in that its inclusion would have “muddied the waters.” The OR booking bureaucracy looks askance (with some justification) at claims that appendicitis needs an OR immediately, but the opportunity to benchmark more serious/urgent conditions against perforated appendicitis was lost.
Oral Antibiotics for Treatment of Uncomplicated Appendicitis
Selänne L, Haijanen J, Sippola S, et al. Three-year outcomes of oral antibiotics vs intravenous and oral antibiotics for uncomplicated acute appendicitis: a secondary analysis of the APPAC II randomized clinical trial. JAMA Surg. 2024;159(7):727-735. doi:10.1001/jamasurg.2023.5947
Summary: In the short term, uncomplicated acute appendicitis (uAA) can be treated successfully with oral (PO) antibiotics alone, but long-term results are lacking. This secondary analysis of a predefined three-year follow-up of the APPAC II (Appendicitis Acuta II) noninferiority randomized clinical trial (Sippola et al, doi:10.1001/jama.2020.23525) compared PO moxifloxacin (400 mg PO daily; n=301) with combined IV ertapenem (1 g/day x 2 days plus PO levofloxacin 500 mg PO daily and metronidazole 500 mg PO three times daily [n=298]) to treat uAA. The primary end point was treatment success at three-year follow-up (resolution of AA and hospital discharge with no AA recurrence, or need for surgical intervention. The secondary end points included appendicitis recurrence after one year, as well as treatment-emergent adverse events, quality of life, length of hospitalization, and length of sick leave. In all, 582 of 599 patients (97%) were available for three-year follow-up. Treatment success rates were 63.4% after PO (95% CI, 58.8% to 8) compared with 65.2% after combined IV/PO therapy (95% CI, 60.5% to 8) (P=0.14 for noninferiority). There were no differences in any secondary end points.
Commentary: These findings should not be interpreted as good news for nonoperative management (NOM) of uAA. PO antibiotics were not noninferior. Prior analysis has shown that NOM is only cost-effective when PO antibiotics are given on an outpatient basis. Hospitalization for IV antibiotics, even for one day, is not cost-effective. Moreover, as follow-up has lengthened, the failure rate, estimated to be 25% to 30% at one year, appears at three-year follow-up to be at least 40%. This does not bode well for longer-term follow-up. Patients should know this.
This article is from the March 2025 print issue.




Please log in to post a comment