
Pneumonia and Other Risks of Proton-Pump Inhibitors in Critical Illness
Palmowski L, von Busch A, Unterberg M, et al. Timely cessation of proton pump inhibitors in critically ill patients impacts morbidity and mortality: A propensity score-matched cohort study. Crit Care Med. 2024;52(2):190-199. doi: 10.1097/CCM.0000000000006104.
Summary: A nationwide retrospective cohort study of patients treated with proton-pump inhibitors (PPIs) in German intensive care units (ICUs) during 2017-2018 was conducted to test the hypotheses that non-indicated PPI therapy continued beyond hospital discharge is associated with increased morbidity, rehospitalization, and mortality. A total of 591,207 patient datasets from a German healthcare insurance database were screened. There were 11,576 patients who received first-time PPI therapy during their index ICU stay without an indication for its continuation. All patients had a minimum two-year follow-up. Groups were compared who received no further PPI therapy post-discharge and who had continuation of PPI beyond eight weeks post-discharge. Frequency of PPI-related adverse events, one-year rehospitalization, and two-year mortality rates were determined. Of the patients, 41.7% (4,825 patients) had PPI therapy continued without an indication. Those patients had a higher risk of pneumonia (odds ratio [OR], 1.27; 95% confidence interval [CI], 1.15-1.39; P<0.001) and cardiovascular events (OR, 1.17; 95% CI, 1.08-1.26; P<0.001). Continued PPI therapy was associated with higher risks of rehospitalization (OR, 1.34; 95% CI, 1.23-1.47) and mortality (hazard ratio [HR], 1.17; 95% CI, 1.08-1.27; P=0.006).
Commentary: PPIs (or histamine-2 antagonists) are prescribed to ICU patients to prevent stress-related gastric mucosal hemorrhage, a.k.a. “stress gastritis.” Combined with better nutritional support, they are undeniably effective as prophylaxis; stress gastritis essentially disappeared three decades ago. The drugs are inexpensive, interchangeable, and widely believed to be safe (harmless?), so prescribing is ubiquitous. In fact, most patients in the ICU don’t need such protection, absent severe traumatic brain injury, burns, coagulopathy, or prolonged mechanical ventilation. These data demonstrate that unnecessary continuation of PPI prophylaxis adversely impacts morbidity and mortality. For at-risk patients, acid-reduction prophylaxis should be short-term. To avoid potentially harmful overuse of PPIs, timely cessation must be ensured. What does “timely” mean? Toleration of oral or enteral feeding would be a reasonable stopping point.
Are Sterile Gloves Necessary for Suture Repair of Lacerations?
Hamem Y, Ayesh H, Asad D, et al. Sterile vs. nonsterile gloves for the repair of wounds and lacerations: A systematic review and meta-analysis. JAMA Surg. 2024;159(2):225-227. doi: 10.1001/jamasurg.2023.5814.
Summary: The aim of this systematic review and meta-analysis of randomized clinical trials (RCTs) was to evaluate the effect of using non-sterile vs. sterile gloves for the repair of lacerations and wounds (minor surgical procedures in emergency, primary care, and outpatient settings) on surgical site infection (SSI) rates. Extracted data included characteristics of studies’ settings, geography, population, wound characteristics, intervention, comparator, and outcomes. The risk of bias was assessed using the Cochrane Risk of Bias 2 tool, and evidence quality was rated using the Grading of Recommendations Assessment, Development and Evaluation (GRADE) tool. Meta-analyses calculated risk ratios (RR) and 95% confidence intervals using random-effects models. The primary outcome was SSI risk. Secondary outcomes included cost and cosmesis. Six RCTs (6,182 patients) were identified, but only one was conducted in a low-income country. Three studies were conducted in emergency settings. Most studies reported the use of other sterile techniques, including disinfectants and sterile instruments. Three studies were judged to be at high risk of bias. Four studies that evaluated the effect of glove sterility on the SSI rate for wound repairs found no difference in the incidence of SSI (RR, 1.17; 95% CI, 0.88-1.55; P=0.62). Analysis by type of repair (trauma vs. dermatologic/plastic excision and repair) was consistent for the use of non-sterile gloves (RR, 1.17; 95% CI, 0.89-1.55; P=0.26).
Commentary: Practice guidelines based on common sense recommend sterile gloves during minor procedures to prevent SSIs. However, no clear evidence suggests that non-sterile gloves are less effective. This is a first step on the path to that evidence; more data are needed. In resource-limited health care settings, it is crucial to consider the cost effectiveness of health care interventions. Sterile gloves are but one such intervention for wound repair; perhaps wound preparation and sterile instrumentation and dressings are more important. Obviation of the need for sterile gloves in simple wound repair would have tremendous implications for care in low-resource settings and austere conditions, and possibly everywhere.
Disparities in SSI Risk
Ngo L, Quintero L, Parreco JP. Nationwide propensity-matched comparison of surgical site infections in safety net hospitals. JAMA Surg. 2024;159(5):588-590. doi: 10.1001/jamasurg.2023.7863.
Summary: The investigators compared rates of SSIs in all patients undergoing gastrointestinal (GI) surgery in safety net hospitals (SNH) vs. all other hospitals using data from the Nationwide Readmissions Database (NRD) for 2019-2020, when International Statistical Classification of Diseases and Related Health Problems, Tenth Revision (ICD-10) code use became prevalent. The primary outcome was SSI identified during the index admission or during readmission within 90 days. SNHs were defined by size, metropolitan locale, public funding, and teaching status. Propensity matching (1:1) considered age, sex, anatomic site of surgery, elective surgery, trauma, low household income, insurance status, and 38 Elixhauser comorbidities. Among 392,368 patients identified, 23,447 (6.0%) were treated in a SNH. Of the total group, 13,264 were female (50.2%); mean [SD] age was 54 [18] years. Matching was successful, with no differences detected between groups. The overall SSI rate was 3.0% (n=11,617), of which 59.2% (n=6,878) were found during readmission. The SSI rate in SNHs was 7.8% (n=911; P<0.01). After matching, the SSI risk was increased in SNHs (OR, 1.29; 95% CI, 1.16-1.42; P<0.01), and was consistent across SSI subtypes (superficial incisional: OR, 1.27; 95% CI, 1.07-1.52; deep incisional: OR, 1.76; 95% CI, 1.16-2.71; organ-space: OR, 1.30; CI, 1.12-1.51) (P<0.01 for all).
Commentary: The Centers for Medicare & Medicaid Services (CMS) imposed financial penalties on hospitals with high rates of health care–associated infections beginning in 2014 (and rewarded hospitals with low rates), but the program has been ineffective at reducing infection rates at SNHs, which disproportionately serve medically complex, economically disadvantaged patients who are at higher risk for infection. Study limitations include the challenges of using administrative databases, which are subject to coding errors. Additionally, the NRD does not include data on race and ethnicity, precluding those analyses. Surgeons must be mindful of the existence of these and other disparities, and that they are not remediated by financial incentives and penalties. There is much work to be done.
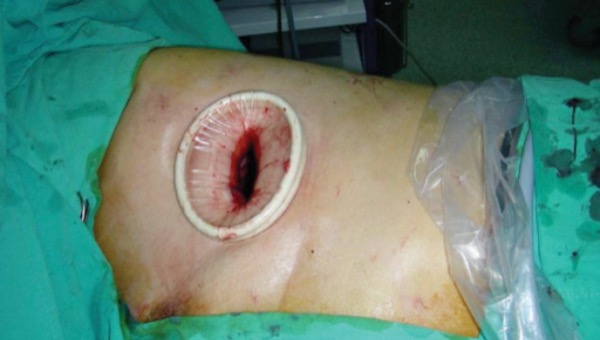
Plastic Wound Protectors for Clean-Contaminated Open GI Surgery
Yoon N, Mun JY, Kye B-H, et al. Plastic wound protector vs. surgical gauze for surgical site infection reduction in open GI surgery: A randomized clinical trial. JAMA Surg. 2024;159(7):737-746. doi: 10.1001/jamasurg.2024.0765.
Summary: This multicenter, single-blind RCT, conducted at 13 academic hospitals, examined the efficacy of a dual-ring plastic wound protector to lower the SSI rate in open GI surgery irrespective of intraabdominal contamination. Patients undergoing open operation (for example, for perforated viscus) were eligible. Patients were randomized 1:1 to the plastic wound protector or conventional surgical gauze (control group) to protect the abdominal wall incision site during surgery. The primary endpoint was SSI within 30 days postoperatively. There were 458 randomized patients; one patient in the control group was excluded, leaving 457 in the intention-to-treat (ITT) analysis. The mean [SD] age was 58 [12] years, 56% were male, and 341 (75%) had a clean–contaminated incision. Length of hospital stay and overall postoperative complication rates were similar between groups. The overall SSI rate (ITT analysis) was 15.7% (72 of 458): 10.9% for the wound protector (25 of 229 patients) compared with 20.5% (47 of 229 patients) for surgical gauze. The wound protector reduced significantly the overall risk of SSI (relative risk reduction [RRR] of 47%; 95% CI, 17%-66%). For clean–contaminated incisions, the SSI rate decreased significantly with the use of the wound protector (RRR, 44%; 95% CI, 4%-67%), particularly for superficial incisional SSIs (RRR, 43%; 95% CI, 7%-64%). The wound protector did not protect against SSIs for contaminated or dirty incisions, or against deep incisional or organ-space SSIs.
Commentary: The overall SSI rate of nearly 16% in this study is consistent with the published literature. High SSI rates, especially for dirty open colorectal surgery (around 30%) are alarming but not surprising. The finding that intraoperative use of a plastic wound protector reduced superficial incisional SSI after clean–contaminated open abdominal GI surgery is consistent with multiple recent guideline recommendations for their use. The study was not powered for analysis of contaminated or dirty operations, or for (less-common) deep incisional or organ-space infections, so several questions remain to be answered. A strength of the study was the mandatory adherence to an SSI prevention bundle (mechanical bowel preparation, prophylactic antibiotic, surgical field antisepsis, and intraoperative maintenance of normothermia). Incisional irrigation was with normal saline rather than an antibiotic solution. However, replacement of surgical gowns and gloves was at the discretion of the operating surgeon, and no mention was made of a separate instrument tray for closure. Additionally, no specific wound dressing type was mandated.
Silver-Impregnated Wound Dressings for Prevention of SSI
Kosugi C, Koda K, Shimizu H, et al. A randomized trial of ionic silver dressing to reduce surgical site infection after gastrointestinal surgery. Ann Surg Open. 2024;5(1):e402. doi: 10.1097/AS9.0000000000000402.
Summary: A single-center, randomized (1:1) open-label RCT was conducted to determine if sodium carboxymethylcellulose dressings containing 1.2% ionic silver (study group) were superior to semipermeable film dressings (control group) for preventing superficial incisional SSIs in patients undergoing elective GI surgery with an incision length of >4 cm. Emergency operations and incisions left open were excluded. The dressing was left in place for 48 hours after surgery. The primary endpoint was SSI within 30 days after surgery. There were 865 patients (427 in the study group, 438 controls) who were qualified for analysis of the primary endpoint. Only 22% of the patients underwent upper GI surgery. About 50% of patients underwent laparoscopic surgery. Superficial SSIs were significantly less common in the study group than in controls (6.8% vs. 11.4%; P=0.019). The rate of superficial incisional SSI was significantly lower in the study group for patients undergoing lower GI surgery (P=0.042), but there was no difference after upper GI surgery. Multivariable analysis identified dressing type as an independent factor for reducing superficial incisional SSIs (OR, 0.602; 95% CI, 0.367-0.986; P=0.044).
Commentary: Multiple clinical trials have assessed the effectiveness of silver-containing dressings, but, heretofore, systematic reviews have found insufficient evidence to indicate that silver-impregnated dressings prevent SSI. This study does not change the situation. Silver dressings reduced superficial SSIs compared to film dressings only after lower GI surgery. This study did not meet its primary endpoint because efficacy for lower GI surgery was not prespecified. Making the study even more difficult to interpret, all patients received antibiotic prophylaxis for two to three days (cefazolin for two days for upper GI surgery, and flomoxef [an oxacephem usually classified as a second-generation cephalosporin] for three days for lower GI surgery), as is customary in Japan. Moreover, the indications to restart antibiotics in the postoperative period included fever (>38° C) or leukocytosis, which also differ from North American practice.
This article is from the August 2024 print issue.




Please log in to post a comment